The UK Health Security Agency (UKHSA) has warned parents and carers to be alert after an increase in Strep A infections across the country. But what exactly are Strep A infections and what are the warning signs?
You should call 999 or go to A&E if:
- your child is having difficulty breathing you may notice grunting noises or their tummy sucking under their ribs
- there are pauses when your child breathes
- your child’s skin, tongue or lips are blue
- your child is floppy and will not wake up or stay awake
- is pale, mottled and feels abnormally cold to touch
- Has blue lips
- Too breathless to talk / eat or drink
- Has a fit/seizure
- Is extremely agitated (crying inconsolably despite distraction), confused of very lethargic (difficult to wake)
- Has dark green vomit
- Has a rash that does not disappear with pressure (the ‘Glass Test‘)
You should contact NHS 111 or your GP if:
- s finding it hard to breathe
- Has laboured/rapid breathing or they are working hard to breathe – drawing in of the muscles below their lower ribs, at their neck or between their ribs (recession).
- Unable to swallow saliva
- Has features suggestive of scarlet fever
- Seems dehydrated (sunken eyes, drowsy or not passed urine for 12 hours)
- Is drowsy (excessively sleepy) or irritable (unable to settle them with toys, TV, food or picking up) – especially if they remain drowsy or irritable despite their fever coming down
- Has extreme shivering or complains of muscle pain
- Has a painful, red swollen gland in their neck which is increasing in size
- Is 3-6 months of age with a temperature of 39°C/102.2°F or above (but fever is common in babies up to two days after they receive vaccinations)
- Continues to have a a fever of 38°C or above for more than 5 days
- If your child has recently had scarlet fever but now appears to have a puffy face/eyelids, tea ‘coca-cola’ coloured urine (pee), or a swollen, painful joint(s)
- Is getting worse or if you are worried
If none of the above features are present:
Continue providing your child’s care at home. If you are still concerned about your child, speak to your health visitor, local pharmacist or call NHS 111– dial 111
Children and young people who are unwell and have a high temperature should stay at home. They can go back to school, college or childcare when they no longer have a high temperature, and they are well enough to attend.
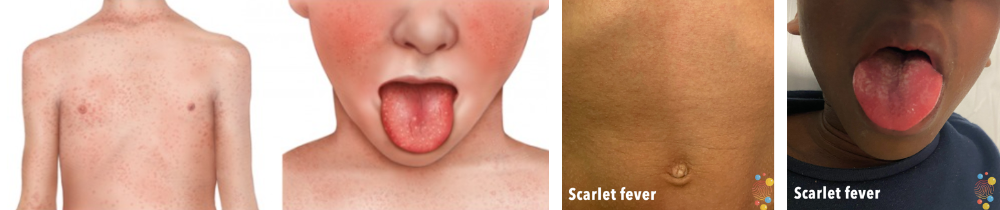
The rash of scarlet fever often begins with small spots on the body that then spread to the neck, arms and legs over the next 1-2 days. It is often ‘sand-paper’ like to touch but is not itchy.
Your child may also have a:
- Sore throat/tonsillitis
- Fever (temperature of 38°C (100.4°F) or above)
- Painful, swollen glands in the neck
- A red tongue (strawberry tongue)
What should you do?
- If you think your child has scarlet fever, they should be seen by their GP. They may need treatment with antibiotics.
- To make your child more comfortable, you may want to lower their temperature using paracetamol (calpol) and/or ibuprofen. Use one and if your child has not improved 2/3 hours later you may want to try giving the other medicine. However, remember that fever is a normal response that may help the body to fight infection and paracetamol/ibuprofen will not get rid of it entirely.
- Avoid tepid sponging your child – it doesn’t actually reduce your child’s temperature and may cause your child to shiver.
- Encourage them to drink plenty of fluids.
- Good hand and respiratory hygiene are important for stopping the spread of many bugs. By teaching your child how to wash their hands properly with soap for 20 seconds, using a tissue to catch coughs and sneezes, and keeping away from others when feeling unwell, they will be able to reduce the risk of picking up or spreading infections. So remember to:
- Catch it: always cough or sneeze into a tissue
Bin it: always throw the used tissue in a bin
Kill it: always wash your hands with soap and hot water
- Catch it: always cough or sneeze into a tissue
How long will your child’s symptoms last?
- The sore throat and fever often last for about 3-6 days and the rash usually improves within a week. Antibiotics reduce the length of fever/sore throat by about 1 day.
- Children commonly experience peeling of their fingers and toes after scarlet fever.
- Your child is no longer infectious to others (contagious) after 24 hours of starting antibiotics and can go back to school/nursery if they feel well enough.
What is Strep A?
Strep A is a bacteria that is sometimes found in the throat or on the skin that can cause a range of illnesses, including strep throat and impetigo. Strep A can also cause scarlet fever, as well as a much rarer illness called invasive Group A Strep (iGAS).
What is scarlet fever?
Scarlet fever is a contagious infection that mostly affects young children. It is usually mild and can be treated with antibiotics but spreads very easily.
The symptoms of scarlet fever are a sore throat, headache and high temperature along with a fine body rash with a sandpapery feel. The rash normally starts on the chest and tummy and then spreads. It will normally look pink or red on pale skin but may be harder to see on darker skin, though you will still be able to feel it.
Another symptom is a white coating on the tongue which peels, leaving the tongue red, swollen and covered in little bumps (‘strawberry tongue’).
What should I do if I suspect my child has scarlet fever?
If you think your child may have scarlet fever, you should contact NHS 111 or your GP so that they can start a course of antibiotics as soon as possible. This is important because early treatment of scarlet fever with antibiotics reduces the risk of complications such as pneumonia or a bloodstream infection.
If your child is confirmed as having scarlet fever, you should keep them at home until at least 24 hours after the start of antibiotic treatment to avoid spreading the infection to others..
What is invasive Group A Strep?
Invasive Group A Strep or iGAS is a very rare illness caused by Strep A bacteria getting into the bloodstream. While this illness is still very uncommon, there has been an increase in cases this year compared to the pre-pandemic period. UKHSA advises parents and carers to talk to a health professional if their child is showing signs of deteriorating after a bout of scarlet fever, a sore throat, or a respiratory infection.
Further information on scarlet fever is available on the NHS website. More information on strep A infections, including both scarlet fever and iGas, is available on the UKHSA website